India’s battle with malnutrition once revolved around scarcity. Today, it is increasingly defined by excess—and the shift is both rapid and alarming. The latest intervention by the Indian Council of Medical Research underscores this transformation, as it raises a nationwide alarm over the country’s growing obesity burden.
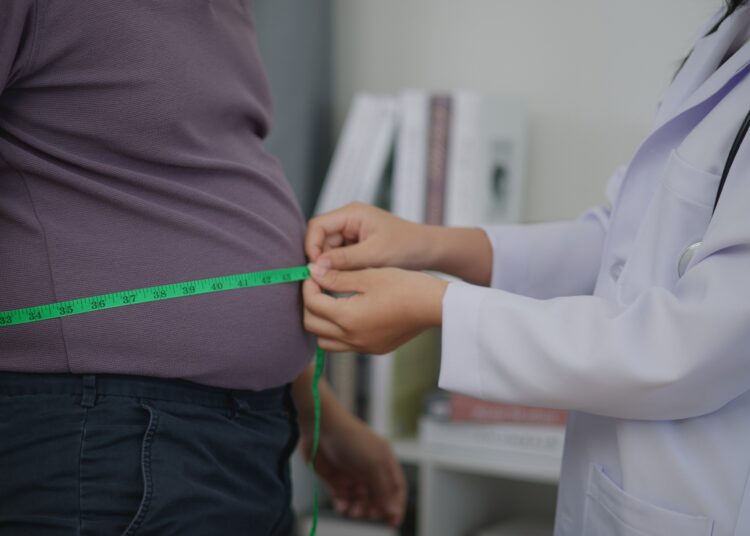
At the heart of this concern lies a stark statistic: nearly one in four Indian adults is now overweight or obese. What was once perceived as an urban lifestyle issue has quietly permeated deeper into the social fabric, cutting across geographies, age groups, and income levels.
Recognising the scale of the problem, ICMR has initiated a nationwide exercise aimed at identifying what truly works in reducing weight and associated health risks. This is not merely another awareness campaign—it is an attempt to build a scientific, evidence-based framework tailored to Indian bodies, diets, and lifestyles.
The urgency is well-founded. Obesity is no longer an isolated condition; it is a gateway to a spectrum of non-communicable diseases. From diabetes and cardiovascular disorders to metabolic syndromes, the expanding waistline has become a visible marker of deeper, systemic health risks. Research increasingly points to abdominal fat—not just overall body weight—as a critical predictor of disease, particularly in the Indian population where metabolic vulnerabilities emerge earlier.
What makes the situation more complex is the nature of its drivers. Rapid urbanisation, sedentary lifestyles, the proliferation of ultra-processed foods, and shifting dietary habits have collectively altered how India eats, works, and lives. The consequences are now manifesting not just in adults but in children as well, raising concerns about a generational health crisis in the making.
ICMR’s response reflects a broader shift in public health thinking—from reactive treatment to proactive prevention. By seeking to establish clear, research-backed strategies, the initiative aims to bring coherence to how obesity is diagnosed, managed, and prevented across the country. It also signals the need for culturally relevant solutions, rather than imported frameworks that may not align with Indian realities.
Yet, the challenge extends beyond policy and research. Obesity, unlike many other health conditions, is deeply intertwined with behaviour, environment, and social norms. Tackling it will require more than clinical guidelines—it will demand sustained lifestyle changes at the individual and community levels.
In that sense, ICMR’s “belly alarm” is less a warning and more a turning point. It reframes obesity from a matter of personal responsibility to a collective public health priority—one that India can no longer afford to ignore.